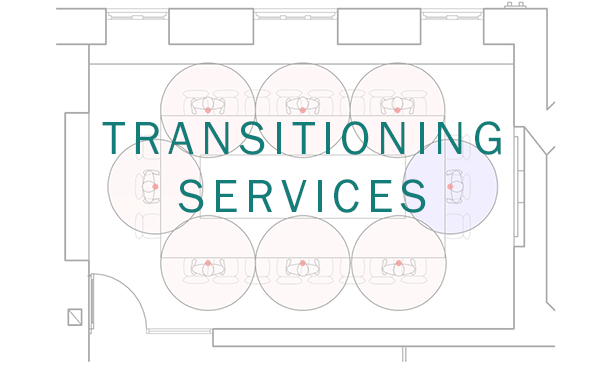
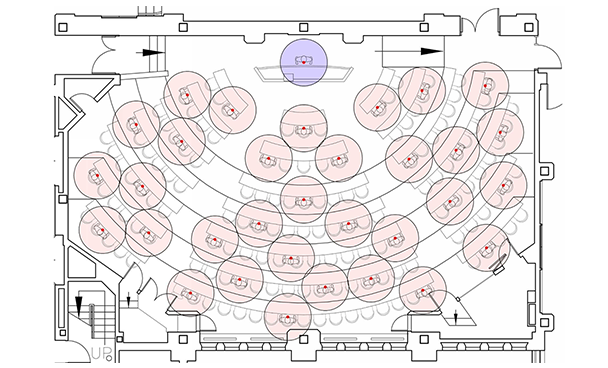
For a good part of this pandemic here in the Northeast US, we have had plentiful outdoor recreational opportunities and have been able to socialize with others safely outdoors. However, in true Game of Thrones fashion, winter is coming, and with no vaccine on the near horizon we will have to figure out how to safely function and interact indoors.
Case studies show that SARS-CoV-2 (the term for the virus) is airborne and transmitted through aerosols[i]. Very recently scientists were able to detect active virus in the air up to 15ft away from patients in a hospital setting.[ii] Fortunately, we have a lot of data now that show wearing masks/ face coverings is effective in reducing the risk of transmission of COVID-19 (the term for the disease).[iii] [iv] Interestingly, in addition to reducing the risk of transmission to others, wearing a mask also provides some protection to the wearer, and experts also think that it can reduce the severity of the disease if it is acquired.[v]
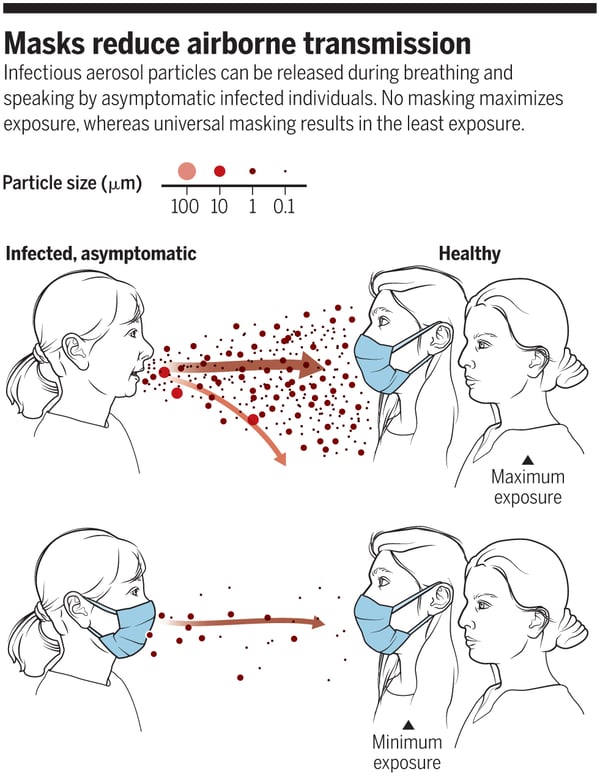
Copyright © 2020, American Association for the Advancement of Science [vi]
All of the built environment measures we can implement rely on universal mask wearing by indoor occupants. In interior spaces, we rely on masks as source control to reduce the amount of virus being introduced to the air but it is important to note that masks are not a substitute for physical distancing. Although masks reduce risk, they are not 100% effective, which is why using multiple measures to reduce risk is a more effective strategy than relying on just one measure.
Here are some considerations when selecting a mask.
1. N95 AND SURGICAL FACE MASKS
N95 respirators are the most effective and have been tested to achieve a very close facial fit and 95% filtration of airborne particles in a laboratory setting[vii]. Interestingly, N95 respirators actually perform better in the real world. Although, please note that half of Chinese-made N95 and KN95 masks failed quality tests.[viii] [ix]
Surgical masks are not regulated for fit or for respiratory protection, but they have been shown to perform very well.[x] [xi] Note that since these qualities aren’t regulated, the fact that certain surgical masks have tested well doesn’t guarantee that all of them perform well.

Image source: CDC
The CDC is currently recommending that both of these masks be reserved for healthcare workers and other medical first responders and recommends the use of cloth face coverings for the general public.[xii] Although cloth masks are less effective than certified masks, they can effectively reduce risk.[xiii] Though N95 and surgical mask production has increased with the rise in cases in the United States, there are still PPE (Personal Protective Equipment) shortages[xiv]. As a result, we recommend not buying any new disposable PPE, but if you already have an opened box, consider reusing them as recommended below.
2. CLOTH MASK FABRIC
The filtration efficiency of cloth masks is dependent upon the fabric. Typically, more than one layer of a closely woven cotton or canvas is recommended for a homemade face mask.[xv] [xvi] There are plenty of sources for DIY mask patterns, even from the CDC.[xvii] If purchasing your cloth mask, avoid antimicrobial fabrics. Antimicrobials have limited benefit, if any. They can produce antibiotic resistant bacteria, and are associated with developmental, hormonal, and reproductive problems.[xviii]
Laura and her daughter, Kira sprang into action in March and made a total of 60 masks for donation from old shirt fabric and elastic bands.

3. MASK FIT
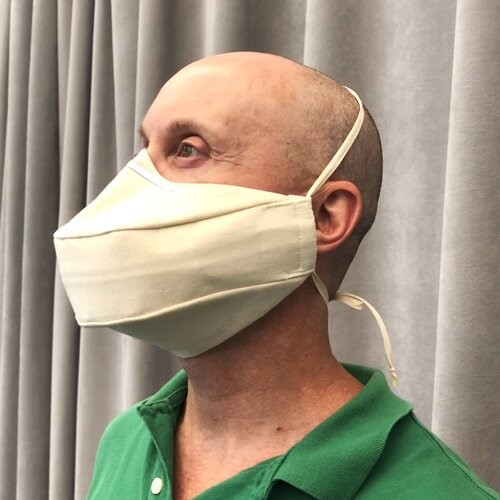
Proper fit is critical to prevent air from bypassing the fabric filter of the mask. My unscientific personal test for the fit of my mask is whether it puffs up and down when I breathe.
Bonus: The media has been citing a study recently claiming that gaiters are less effective than wearing no mask at all. In reality, the study’s main purpose was to study a methodology for testing masks, so it was not designed to produce scientifically accurate data about the masks themselves.[xix] A leading aerosol scientist, Linsey Marr, conducted her own test and found that they perform similarly to cloth masks and very well if doubled over.[xx]
4. EXHALATION VALVE
The general recommendation is to avoid using a mask with an exhalation valve[xxi] because it can release more particles than a non-valve mask. Recall that we are currently using masks to prevent particles from escaping the mask in addition to protecting the wearer from particles in the ambient air.[xxii]
5. OCULAR TRANSMISSION
While COVID-19 can be transmitted through the eyes, if properly distanced from potential infection sources ocular transmission is thought to be less likely than through the nose or mouth.[xxiii] If you expect to be within 6ft of someone who may be infected, then protecting your eyes is more important because a direct respiratory droplet can land in your eye. It is also very important not to touch your eyes with unwashed hands. Face shields can protect against ocular transmission, but not against aerosols, so they are not recommended for use in interior spaces without masks.[xxiv]
6. MASK REUSE
Like us you are probably concerned about resource efficiency and waste reduction. Unfortunately, disposable PPE such as N95 respirators and surgical masks are causing excessive waste and pollution.[xxv] These masks are typically made from polypropylene which makes them a form of plastic waste, so we want to avoid using these as a single-use item. Ideally one would have multiple cloth masks that can be washed between uses. We think one article’s recommendation to students is particularly helpful and relatable. “Think of face coverings like underwear – have several pairs, wash them often and don’t share.”[xxvi]
If like me you prefer the fit and lightness of a surgical mask, there is some good news. Although the manufacturers do not advise multiple uses for these items, there is some data that it is safe to reuse single-use PPE, in the same way you can sometimes still eat food safely past its expiration date. In fact, unless they become soiled, they can remain effective for days or weeks.[xxvii] Do not sanitize them with alcohol because that degrades their performance[xxviii] or microwave them because it is dangerous.[xxix] The best guidance is that you have a few of them handy, that you avoid touching the outside surface,[xxx] and that you store them for up to 72 hours between uses in a clean dry well-ventilated space.[xxxi] Also, although it seems like a good idea to store your mask in the sun because it kills the virus, unfortunately it also degrades the mask material.[xxxii]
7. SPECIAL FACE COVERING APPLICATIONS
There are many innovative masks that have appeared to address specialized needs of certain applications. For instance, we know from transmission case studies[xxxiii] that singing is a riskier activity than breathing or talking because singers exhale and inhale a larger volume of air from deeper in the lungs.
The Singer’s Mask was developed by singers FOR singers by Broadway professionals to help contain droplets while allowing space around the mouth to sing comfortably.
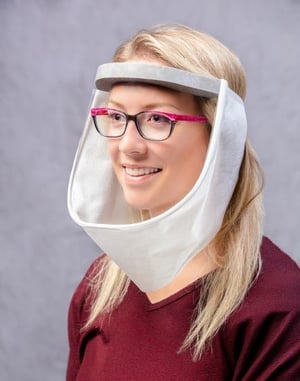
The Humanity Shield allows wearers to prevent the spread of respiratory droplets, while allowing visibility of facial expressions and lip movements for speech perception. This solution is currently all the buzz amongst teachers. Unfortunately, it doesn’t look like it has a good seal at the bottom, so it protects against droplets but not against aerosols, and therefore, we would not recommend it for interior spaces.

There are even masks fashioned for musical instruments. [xxxiv]

Although there is still some confusing and possibly contradictory information, there is NO DOUBT that masks are an EFFECTIVE and NECESSARY part of managing the spread of this disease. At Pirie Associates, we also consider mask-wearing an act of kindness. It is a signal that you are looking out for the health of others.

Even though wearing a mask outdoors is not as critical as indoors, here I am after a bike ride during a heat wave - all geared up for safety - including a mask - showing solidarity. We’re all in this together!
Look out for future installments on the theme of safely returning to interior spaces where we talk about other immediate measures that can be taken to reduce risk indoors.
[i] Coronavirus drifts through the air in microscopic droplets – here’s the science of infectious aerosols
[ii] Viable SARS-CoV-2 in the air of a hospital room with COVID-19 patients
[iii] Face Masks Really Do Matter. The Scientific Evidence Is Growing.
[iv] Yes, Wearing Masks Helps. Here's Why
[v] One more reason to wear a mask: You'll get less sick from COVID-19
[vi] Reducing transmission of SARS-CoV-2
[vii] FDA - N95 Respirators, Surgical Masks, and Face Masks
[viii] Half of Chinese N95 Masks Fail Quality Checks
[ix] Low-Quality Masks Infiltrate U.S. Coronavirus Supply
[x] N95 Masks vs. Surgical Masks: Which Is Better at Preventing the Coronavirus?
[xi] Surgical mask vs N95 respirator for preventing influenza among health care workers: a randomized trial
[xii] CDC - Considerations for Wearing Masks
[xiii] Professional and Home-Made Face Masks Reduce Exposure to Respiratory Infections among the General Population
[xiv] America is running short on masks, gowns and gloves. Again.
[xv] The Ultimate Guide to Homemade Face Masks for Coronavirus
[xvi] What To Look For In A Face Mask, According To Science
[xviii] Antimicrobials, are they helping us or harming us?
[xix] For All We Know, Gaiter Masks Are Fine
[xxi] FDA - N95 Respirators, Surgical Masks, and Face Masks
[xxii] Face masks with valves or vents do not prevent spread of the coronavirus, CDC says
[xxiii] Coronavirus FAQs: Can I Catch It Through My Eyes? Will Goggles Help?
[xxiv] What kind of mask should I be wearing to protect against COVID-19?
[xxv] Coronavirus is causing a flurry of plastic waste. Campaigners fear it may be permanent
[xxvi] Managing Pandemic Health Risks on College Campuses
[xxvii] How Long Do N95 Masks Last? New Data
[xxviii] Sanitizing Masks with Alcohol Degrades Performance
[xxix] Does Microwaving Masks Disinfect Viruses?
[xxx] Reusing face masks: How to remove, clean and store them safely
[xxxi] The Best Way to Disinfect Masks Without Destroying Them
[xxxii] FAQ: How to care for your face mask (and why you shouldn’t hang it from your rear-view mirror)
[xxxiii] High SARS-CoV-2 Attack Rate Following Exposure at a Choir Practice
[xxxiv] Can singing and wind instruments be made safe during coronavirus?